The first, initial test is a simple examination known as a digital rectal examination. This is an examination of the lower rectum that the specialist performs on the patient to examine the prostate area.
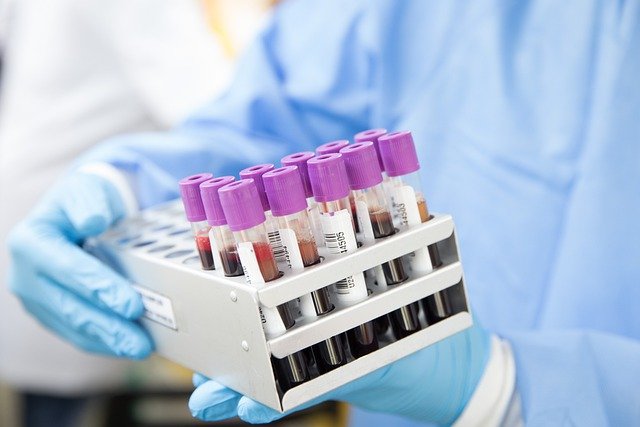
Prostate-specific antigen, or PSA, is a protein produced by normal cells as well as malignant cells in the prostate gland. The PSA test measures the concentration of PSA in a man’s blood. It is obtained by a conventional blood test. If the PSA is over 3ng/ml, a urinalysis and culture will be performed. After ruling out a urinary tract infection, a second PSA test is performed, and if it is over 3ng/ml again, a multiparametric MRI is carried out.
If the blood test shows PSA levels greater than 3ng/ml, a multiparametric MRI is performed. This is a radiological test that provides information about the shape of the prostate from all angles, and also about the surrounding and neighbouring organs and the way they function together.
Based on the results of the above procedures, the Uro-radiology Committee discusses the appropriateness of performing a transrectal or transperineal prostate biopsy using software that can fuse MRI and ultrasound imaging results, or a mapping biopsy.